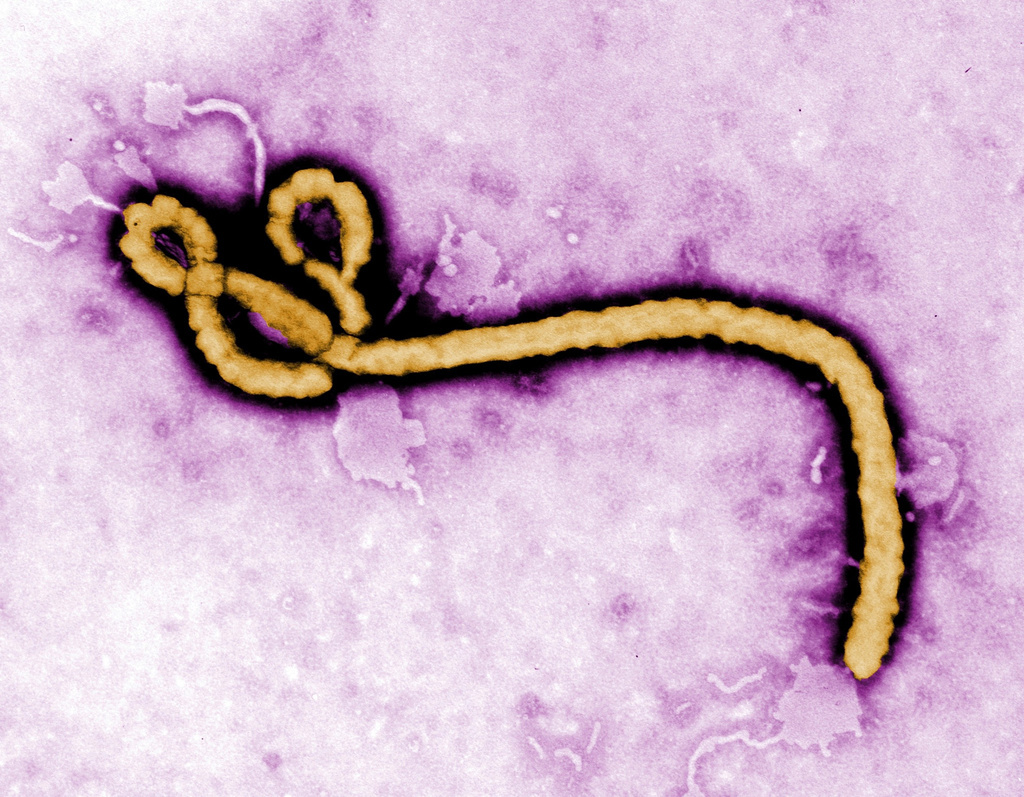
The World Health Organization just dropped the curtain on another global health emergency. The headlines are doing exactly what they always do: counting the bodies, breathing a sigh of relief, and pretending the bureaucratic machinery worked. They point to a localized outbreak, cite a double-digit death toll, and treat the official declaration rollback as a victory for global biosecurity.
It is a total illusion.
The media operates on a simple, flawed premise: an official "emergency" status correlates with actual, systemic threat. It does not. The declaration of a Public Health Emergency of International Concern (PHEIC) has become a political tool and a lagging indicator. By the time the committees convene, argue over wording, and issue a press release, the real trajectory of a pathogen is already locked in.
Treating these bureaucratic start-and-stop announcements as the definitive metric of global safety is actively making us less prepared for real threats.
The Flaw of the Body Count Metric
Mainstream reporting locks onto immediate casualties. If dozens die, it is a tragedy; if the WHO steps in, it is a crisis; if the declaration ends, the crisis is over. This is fundamental risk illiteracy.
In epidemiology, raw mortality during an active outbreak is often a lagging, distorted variable. A pathogen that kills 50 people in an isolated rural hub with zero transport links is tragic, but it is a minor systemic risk. Conversely, a highly transmissible, asymptomatic respiratory virus with a 0.1% mortality rate circulating silently in a major aviation hub is a catastrophic global threat.
The competitor pieces focus entirely on the former because it provides an easy narrative arc. They mistake localized severity for global risk. When you evaluate biosecurity through the lens of body counts alone, you miss the structural vulnerabilities that actually cause pandemics: surveillance gaps, broken supply chains, and regulatory inertia.
Epidemiologist Geoffrey Rose famously established the sick individuals versus sick populations paradigm. If we only look at the extreme cases—the dozens killed—we ignore the underlying distribution of risk across the entire system. The real danger is not the spark that went out; it is the dry tinder left unmanaged.
The Real Cost of Bureaucratic False Alarms
The WHO operates under the International Health Regulations (IHR). Under these rules, declaring a PHEIC is the loudest alarm they can sound. But when everything is an emergency, nothing is.
We have entered a cycle of panic and neglect. I have watched public health agencies pour millions into rapid-response infrastructure for a headline-grabbing virus, only to mothball those exact systems twelve months later when the political will evaporates.
Consider the real trade-offs of these declarations:
- Resource Diversion: Local healthcare systems in developing nations routinely divert funding from high-mortality endemic killers—like tuberculosis, malaria, and basic infant diarrhea—to satisfy the surveillance mandates of a western-facing PHEIC.
- Economic Whiplash: Preemptive border closures and trade restrictions, often driven by panic rather than data, decimate regional economies, leading to long-term health declines that far outweigh the direct impact of the virus.
- Cry-Wolf Syndrome: Public compliance is a finite resource. When global bodies declare emergencies that fail to manifest as personal threats to the average citizen, credibility burns out.
Imagine a scenario where a local health department spends 80% of its discretionary budget tracking a rare hemorrhagic fever because it is the global "topic of the month," while routine childhood vaccination rates drop by 15%. The net result is not a safer population; it is a net increase in preventable death. That is the trade-off the lazy consensus refuses to calculate.
Dismantling the Premise of the "Safe" Consensus
People looking at these declarations frequently ask the same fundamental questions, but they are working from a broken set of assumptions. Let us look at what people actually ask when these emergencies end, and strip away the corporate health PR.
Does the end of a global emergency mean the virus is mutated to a safer form?
Absolutely not. A pathogen does not negotiate with human committees. The termination of an emergency status usually means the geopolitical friction of maintaining the status has surpassed the utility of the declaration. The virus is likely still circulating, mutating, and killing. The only difference is that the international community has decided the current death rate is economically and politically acceptable.
Can we rely on international bodies to catch the next major outbreak early?
History says no. The structural architecture of international health reporting relies on state self-reporting. Nations are deeply incentivized to hide or downplay outbreaks to protect their tourism, trade, and geopolitical standing. By the time an independent validation occurs and a formal emergency is declared, the window for containment has almost always closed.
Should local health policies align directly with global declarations?
If you run a regional health system and wait for a global body to tell you when to scale up or scale down, you are already failing your population. Effective biosecurity is hyper-local and continuous. It does not turn on and off based on a vote in Geneva.
The Case for Continuous, Cold-Blooded Surveillance
The solution to global health threats is not better emergency declarations. The solution is removing the concept of the "emergency" altogether.
We need to shift from a reactive, crisis-model framework to an adversarial, always-on infrastructure. This means investing heavily in passive, non-invasive surveillance systems that do not rely on political permission slips or doctors filling out case reports.
Wastewater sequencing is a prime example. It does not care about national pride, it does not wait for people to show up at an ICU, and it does not require a press conference. It provides raw, unvarnished genomic data in real time. If a novel variant emerges, the data shows it days or weeks before clinical presentations spike.
We must also acknowledge the brutal downside of this contrarian approach: continuous surveillance is incredibly expensive, technologically demanding, and raises massive data privacy concerns. It requires maintaining a permanent wartime footing for a war that is mostly invisible. It means funding genomic labs that will spend 99% of their time reporting absolutely nothing new. Politically, that is a nightmare sell. Politicians want to fund a ribbon-cutting ceremony for a new pandemic response center during a crisis; they do not want to fund the electricity bill for a quiet sequencing lab during a period of stability.
Stop Watching the Press Releases
The competitor article wants you to feel a sense of closure because a committee signed a piece of paper ending a global emergency. It frames health security as a series of distinct battles with clear beginnings and ends.
This view is obsolete.
Biosecurity is an infinite game. There are no truce agreements, no final victories, and no meaningful declarations of safety. The moment you treat the end of an emergency as a green light to return to business as usual, you create the exact vulnerability the next pathogen will exploit.
Stop looking at the body counts from yesterday's outbreak to determine if you are safe today. The real threat is not the virus that just lost its emergency status; it is the data point we are currently ignoring because it does not fit into a dramatic headline. Turn off the press conferences and look at the infrastructure. If the infrastructure is only funded during an emergency, you are completely unprotected.